Why Invest in a Stool Analysis? Part II
In our previous blog post, we discussed how stool analyses can be helpful in forming effective treatment plans for individuals with GI symptoms. However, the health of our GI tract and microbiome has system-wide effects beyond just digestion. It is possible to have imbalances in the GI tract without having significant GI symptoms. In today’s blog, we will discuss other information/benefits we might glean from a stool analysis and other conditions in which we can utilize stool analyses.
Intestinal Permeability
The intestinal barrier acts like a selective gate controlling what is allowed to enter the bloodstream. A healthy barrier should allow small, digested food particles to be absorbed, but prevent undigested food particles, pathogens, and toxins from entering the bloodstream.
The intestinal mucosal barrier consists of a mucus layer containing anti-microbial factors and underlying epithelial cells held together by tight junctions. In a healthy gut, the microbiota do not interact directly with the epithelial cells. Instead, it is sampled in a controlled manner by special cells located in the gut-associated lymphoid tissue (GALT) located along the intestine.
When the tight junctions of the intestinal barrier become compromised, the space between the epithelial cells becomes wider. This allows larger undigested food compounds, toxins, and bacteria to pass through the GALT and into the bloodstream. We call this “intestinal permeability”. These large proteins interact with the immune cells and promote exaggerated immune responses or inflammation. Lipopolysaccharides (LPS), or endotoxins, are molecules found in the outer membrane of gram-negative bacteria. Intestinal permeability allows more LPS to enter the circulation, which also triggers an inflammatory response.

Autoimmune Diseases
Autoimmune diseases are complex immune-mediated diseases influenced by both genetic and environmental factors. Tolerance refers to the immune system’s ability to be non-responsive to innocuous signals like our own tissues, foods, and commensal bacteria. In autoimmune diseases, the immune system gets confused and loses self-tolerance. Our immune cells no longer distinguish between friend or foe, leading to the destruction of our own tissues.
Microorganisms are one environmental trigger implicated in the development of autoimmune diseases. Both overt and occult infections can trigger a loss of self-tolerance and autoantibody production via molecular mimicry. Molecular mimicry occurs when there are structural similarities (similar amino acid sequences) between pathogens and our own tissues. When the immune system mounts a response to the pathogen, there is cross-reactivity stimulated against the similar host tissues. is a mechanism by which there is cross-activation of autoreactive immune cells due to peptide sequence similarities between pathogen-derived peptides and self-peptides.

An example of an overt infection triggering an autoimmune disease would be developing rheumatic fever after a strep infection. Examples of possible occult infections are Klebsiella and Proteus. These are two types of bacteria that can reside in our GI tract. They might not trigger an acute illness, but they have been implicated in the development of rheumatoid arthritis and ankylosing spondylitis.
Short Chain Fatty Acids

Short-chain fatty acids (SCFA) are created when dietary fiber is fermented by bacteria in the colon. Acetate, propionate, and butyrate are the three most common. Butyrate in particular is important for the gastrointestinal tract because it is the primary energy source for colonocytes and helps to regulate tight junction proteins (barrier function). SCFAs have been shown to have diverse roles in body functions outside of the GI tract as well. They can affect appetite, cardiometabolic health, and the production of lipids and energy.

As we mentioned earlier, Intestinal permeability allows for increased exposure to endotoxin/LPS, which promotes inflammation. This is one possible mechanism contributing to insulin resistance. We call this phenomena, metabolic endotoxemia. Short-chain fatty acids help to normalize intestinal permeability and subsequent LPS exposure. They also alter free fatty acid production and help to normalize blood sugar.
Metabolism & Weight Management
The composition of our microbiome has the ability to affect our metabolism and weight. Obese individuals have been shown to have alterations in the composition of their microbiome when compared to healthy weight controls. The ratio of Firmicutes bacteria to Bacteroides bacteria is higher in the obese population. Leptin is the body’s satiety hormone. It is produced by our fat cells and acts on the hypothalamus to tell our brains we do not need to eat more and can burn calories at a normal rate. Leptin resistance refers to when there are high levels of leptin circulating in the body, but the hypothalamus is not responding to it. Leptin resistance can cause hunger and decrease metabolism. Research has shown that increasing prebiotic intake (healthy fiber for our gut bacteria) increases leptin sensitivity.
Cardiovascular Disease
Higher circulating levels of LPS have been associated with cardiovascular diseases including coronary artery disease and chronic heart failure.
Detoxification/Hormone Metabolism
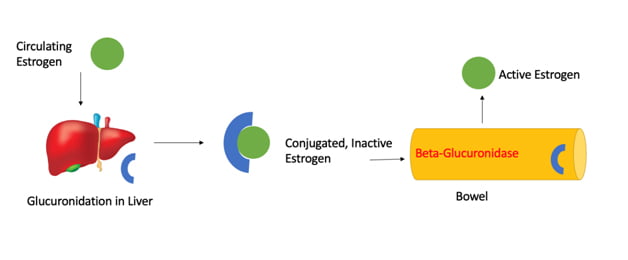
Circulating estrogens are first metabolized in the liver before they can be eliminated from the body. In phase I metabolism in the liver, estrogens undergo hydroxylation (adding an -OH group to the estrogen). These phase I metabolites are still quite reactive though. In phase II metabolism in the liver, the phase I metabolites are inactivated and become water-soluble so they can be eliminated through the kidneys or stool. There are a few different conjugation pathways in phase II metabolism, but one conjugation method is via glucuronidation (adding glucuronic acid). This estrogen glucuronide conjugate can be deconjugated by certain bacterial species in our gut that produce the beta-glucuronidase enzyme. Beta-glucuronidase removes the glucuronic acid from estrogen, allowing it to be reabsorbed into circulation again. This enterohepatic circulation of estrogens can be an underlying cause of estrogen dominant conditions.
When in Doubt, Treat the Gut
Hippocrates once said “All disease begins in the gut.” A stool analysis can be a useful tool for many conditions, beyond just GI complaints. In this blog post, we discussed how intestinal permeability, short-chain fatty acid production, dysbiosis, and certain bacterial species all play a role in inflammation, autoimmune diseases, metabolism, and hormone processing. Let’s take a look at how comprehensive stool analyses can be helpful! All of these snapshots came from a sample report of Genova’s Gi Effects stool analysis.
- SCFA’s:
 We can measure not only the total amount of SCFA’s in the stool but also see the total amount of butyrate. In patients with intestinal permeability and/or insulin resistance + low butyrate, this would provide an opportunity for therapeutic intervention. Butyrate can be given in supplemental form or dietary fiber can be increased to boost butyrate levels.
We can measure not only the total amount of SCFA’s in the stool but also see the total amount of butyrate. In patients with intestinal permeability and/or insulin resistance + low butyrate, this would provide an opportunity for therapeutic intervention. Butyrate can be given in supplemental form or dietary fiber can be increased to boost butyrate levels. - Beta-Glucuronidase:

Beta-glucuronidase is an enzyme produced by certain bacteria in the GI tract. Elevated levels of beta-glucuronidase are associated with an imbalanced intestinal microbiota profile. As we discussed earlier, elevated levels of beta-glucurondiase in the GI tract can affect hormone metabolism, increasing the re-absorption of estrogens. In patients with estrogen dominant conditions or those at risk for hormone-sensitive cancers, this provides a treatment option for us. Rebalancing the gut microbiome and using treatments like indole-3-carbinol allow us to decrease beta-glucuronidase activity in the gut. - Firmicutes:Bacteroides Ratio:
 Comprehensive stool analyses use PCR testing to measure different bacterial species and strains in the GI tract. This gives us the opportunity to not only look at the relative abundance of the various bacteria phyla but also compare the two largest phyla, but also compare the two largest phyla, Firmicutes and Bacteroides (F/B ratio). As we mentioned earlier in this post, a high F/B ratio is associated with metabolic diseases like type 2 diabetes, non-alcoholic fatty liver disease, and high body mass index. Probiotic supplementation with specific strains an increasing beans in the diet are strategies we can implement to increase Bacteroidetes.
Comprehensive stool analyses use PCR testing to measure different bacterial species and strains in the GI tract. This gives us the opportunity to not only look at the relative abundance of the various bacteria phyla but also compare the two largest phyla, but also compare the two largest phyla, Firmicutes and Bacteroides (F/B ratio). As we mentioned earlier in this post, a high F/B ratio is associated with metabolic diseases like type 2 diabetes, non-alcoholic fatty liver disease, and high body mass index. Probiotic supplementation with specific strains an increasing beans in the diet are strategies we can implement to increase Bacteroidetes. - Bacterial Culture for Strains of Interest:

In addition to the PCR testing, the test also cultures live organisms and test their susceptibility to different anti-microbial treatments. If this patient had an autoimmune disease, we would use the culture and sensitivity testing to select an effective anti-microbial treatment to remove the Klebsiella pneumonia. - GI Inflammation // Intestinal Permeability:


Calprotectin and EPX are secreted by immune cells in the GI tract. When they are elevated, it is indicative of GI inflammation. Zonulin is a protein that regulates tight junctions in the GI tract. Elevated inflammation and/or elevated zonulin point to an increased risk of intestinal permeability. In these cases, we would consider mucosal healing protocols and elimination diets.
Schedule a free 15 minute consultation with Dr. Cloyd today to see if a Stool Analysis is the right test for you. Schedule Now

 We can measure not only the total amount of SCFA’s in the stool but also see the total amount of butyrate. In patients with intestinal permeability and/or insulin resistance + low butyrate, this would provide an opportunity for therapeutic intervention. Butyrate can be given in supplemental form or dietary fiber can be increased to boost butyrate levels.
We can measure not only the total amount of SCFA’s in the stool but also see the total amount of butyrate. In patients with intestinal permeability and/or insulin resistance + low butyrate, this would provide an opportunity for therapeutic intervention. Butyrate can be given in supplemental form or dietary fiber can be increased to boost butyrate levels.
 Comprehensive stool analyses use PCR testing to measure different bacterial species and strains in the GI tract. This gives us the opportunity to not only look at the relative abundance of the various bacteria phyla but also compare the two largest phyla, but also compare the two largest phyla, Firmicutes and Bacteroides (F/B ratio). As we mentioned earlier in this post, a high F/B ratio is associated with metabolic diseases like type 2 diabetes, non-alcoholic fatty liver disease, and high body mass index. Probiotic supplementation with specific strains an increasing beans in the diet are strategies we can implement to increase Bacteroidetes.
Comprehensive stool analyses use PCR testing to measure different bacterial species and strains in the GI tract. This gives us the opportunity to not only look at the relative abundance of the various bacteria phyla but also compare the two largest phyla, but also compare the two largest phyla, Firmicutes and Bacteroides (F/B ratio). As we mentioned earlier in this post, a high F/B ratio is associated with metabolic diseases like type 2 diabetes, non-alcoholic fatty liver disease, and high body mass index. Probiotic supplementation with specific strains an increasing beans in the diet are strategies we can implement to increase Bacteroidetes.

